Minimally Invasive Brain Surgery

Kathleen Khu |
Neurosurgery has not traditionally been considered an
area of surgery which could lend itself to minimally invasive
techniques. But minimally invasive brain surgery
(MIBS) has evolved to include small skin incisions, better
illumination, and minimal
disturbance of the normal brain
tissue. The philosophy is to create
as little disruption to the
patient as possible - the clinical
value of minimally disrupting
the patient's tissues is to allow
the patient to recover quickly
and resume his/her normal life
as soon as possible.
Neurosurgical technique has progressed, and advances
in anaesthetic techniques and medical technology, such
as neuronavigation and improved optical devices, have
also played a crucial role in enabling MIBS. There are
also exciting advances in minimally invasive spine surgery
which will revolutionize this area of surgery. Some
exciting examples of MIBS being performed at the
Toronto Western Hospital (TWH) are described below
OUTPATIENT CRANIOTOMY

Mark Bernstein
|
In late 1996, the first awake outpatient
craniotomy in the world
was performed at TWH. Since
then, almost 400 brain tumour
patients have been operated
on, on an outpatient (i.e. Day
Surgery) basis, with low morbidity
and high patient satisfaction.
Awake outpatient craniotomy
with brain mapping has been
found to be a safe and effective procedure for the surgical
treatment of patients with gliomas and metastatic
tumours. The patient is discharged after 6 hours post-op,
assuming a CT done at 4 hours shows no problems and
the patient remains well.
An important adjunct that greatly facilitates outpatient
surgery is the use of image guidance for the localization of brain tumours. With the neuronavigation system,
the location of the tumour is more easily pinpointed,
minimizing disturbance to the normal surrounding
brain and saving operative time. In addition, the skin
incision and the bone flap are smaller and tailored to
expose the lesion, lessening the patient's post-op pain
and discomfort. Many patients report that going home
on the same day makes them feel better overall. They
recover faster at home, within a familiar environment,
giving them more confidence to resume their day-to-day
activities. Outpatient brain surgery is slowly catching
on outside Toronto and represents a major advance in
patient care and patient flow, minimising the use of
shrinking inpatient resources.
KEYHOLE APPROACHES TO ANTERIOR CIRCULATION ANEURYSMS
Aneurysms have traditionally been approached through
large bone flaps. However, the actual working space for
the exposure, dissection, and clipping of anterior circulation
aneurysms is small, so as long as the principles of
minimal brain retraction and proximal vascular control
are followed, patient outcomes after aneurysmal clipping
using small versus large openings are comparable.
Examples of keyhole approaches to anterior circulation
aneurysms include the supraorbital and the micropterional
approach. The former involves a skin incision
above the eyebrow and the latter involves a small curvilinear
skin incision at the temple; in both cases a dollar
coin-sized craniotomy is fashioned. In both approaches,
the aneurysm is dissected and clipped using the usual
microsurgical techniques. Narrower instruments are
needed to fit through the opening without obscuring
the view.
Focused approaches such as these would have less
morbidity since only the relevant structures are exposed.
Smaller incisions heal faster, are aesthetically more pleasing,
and promote faster recovery. Unruptured aneurysms
can be operated on an outpatient basis.
|
ENDOSCOPIC APPROACHES TO SKULL BASE TUMOURS
The majority of sellar tumours have been approached
through the transsphenoidal route for decades, and
tumour resection has traditionally been accomplished
with the use of the operating microscope. Over the past
few years, the endoscope has been introduced initially
as an adjunct to the microscope, until pure endoscopic
techniques have been developed to supplant the microscope.
Expansion of the bony resection results in the
endoscopic endonasal transbasal approach.
The transbasal approach still utilizes the natural corridors
leading from the nasal cavity to the sellar region
of the skull. These tumours are outside the brain so this
approach is ideal in that it allows safe and effective tumour
resection with minimal anatomic disruption of the brain.
The advantage of the endoscopic technique over the
microscopic one is that the former requires no mucosal
incisions, allows a wider and more magnified view of the
operative field, and is able to visualize areas that are outside
a microscope's line of sight. It also rarely requires nasal
packing post-operatively. Overall this technique gives better
visualization of the tumour and causes less patient discomfort
compared to the traditional microscopic approach. The
true advances involve expanding the clinical applications to
remove much larger lesions such as skull base meningiomas
with minimal touching of the brain.
GAMMA KNIFE STEREOTACTIC RADIOSURGERY
Gamma Knife stereotactic radiosurgery (GKSRS) is an
outpatient procedure in which a highly focused dose of
radiation is delivered in a single fraction. It is in reality
a radiation procedure but it was initially developed
and championed almost entirely by neurosurgeons and
many leaders in the field now call it "Gamma surgery".
It allows the treatment of discrete lesions with high comformality
using three-dimensional stereotactic imaging
and the delivery of multiple radiation beams focusing
on the target lesion. The beams are so precise that the
surrounding normal tissue receives minimal radiation.
GKSRS is used to treat a variety of conditions, such
as benign tumours (mainly vestibular schwannoma),
malignant tumours (mainly metastases), vascular lesions
(AVM's), and functional disorders (mainly trigeminal
neuralgia).
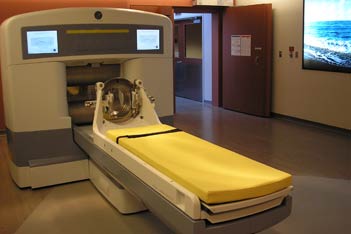
Gamma Knife
On the day of the procedure, a stereotactic frame is
applied on the patient's head and screwed into place.
The patient then undergoes imaging with the frame in
situ. Treatment planning is done, after which the patient
receives the actual treatment. Afterwards, the frame
comes off and the patient can go home after one hour
of observation.
Compared to the surgical alternative, GKSRS is much
less invasive and provides similar success rates. It has
been proven to be a safe and effective mode of treatment,
especially for patients with deep-seated lesions and for
elderly patients with medical co-morbidities who would
have high surgical risks.
Kathleen Khu,
Clinical Fellow in Neurosurgical Oncology,
Toronto Western Hospital
Mark Bernstein,
Professor of Surgery and Neurosurgeon at
Toronto Western Hospital |